What is Breathing Pattern Disorders (BPD)?
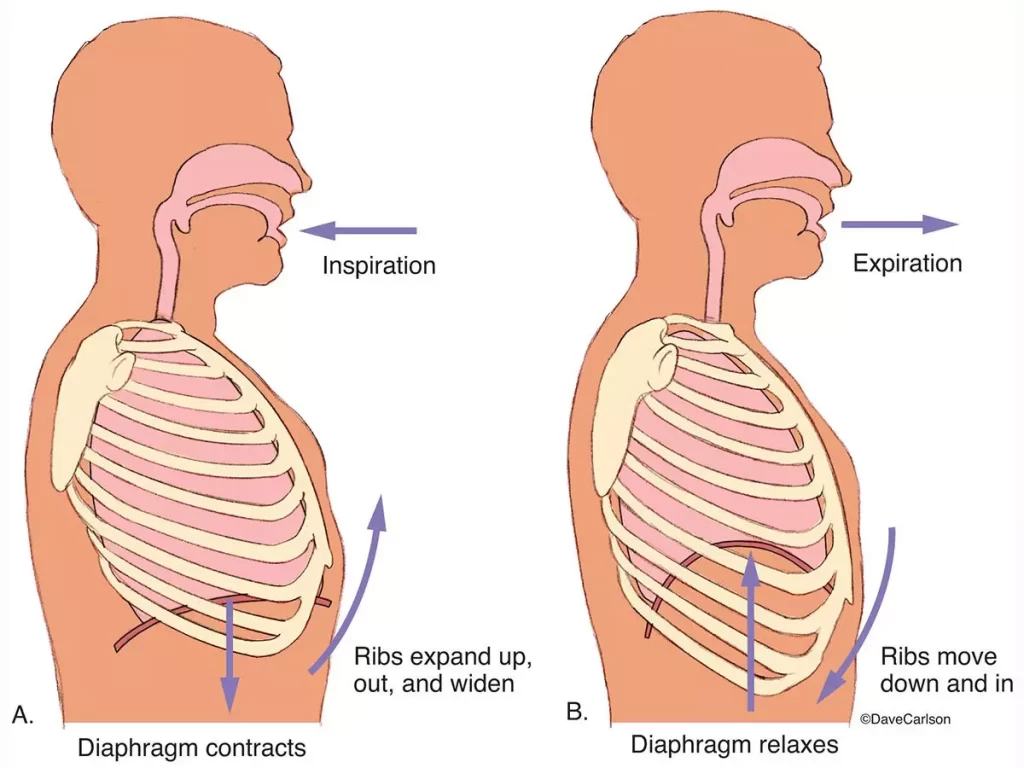
Breathing Pattern Disorders (BPD) or Dysfunctional Breathing are abnormal respiratory patterns specifically related to over-breathing. They range from simple upper chest breathing to at the extreme end of the scale, hyperventilation (HVS).
Dysfunctional breathing (DB) is defined as chronic or recurrent changes in the breathing pattern that cannot be attributed to a specific medical diagnosis, causing respiratory and non-respiratory complaints. It is not a disease process, but rather alterations in breathing patterns that interfere with normal respiratory processes. BPD can, however, co-exist with diseases such as Chronic Obstructive Pulmonary Disease or heart disease.
BPDs or dysfunctional breathing can destabilise mind, muscles, mood, and metabolism. They can play a part in for instance premenstrual syndrome, chronic fatigue, neck, back and pelvic pain, fibromyalgia, and some aspects of anxiety and depression.
Around 10% of patients in a population are diagnosed with hyperventilation syndrome. However, many more people have subtle, yet clinically significant, breathing pattern disorders. Dysfunctional breathing is more prevalent in women (14%) than in men (2%). Little is known about dysfunctional breathing in children. Preliminary data suggest 5.3% or more of children with asthma have dysfunctional breathing and that, unlike in adults, it is associated with poorer asthma control.
Causes of Breathing Pattern Disorders (BPD)?
Breathing pattern disorders occur when ventilation exceeds metabolic demands, resulting in symptom-producing hemodynamic and chemical changes. Habitual failure to fully exhale – involving an upper chest breathing pattern may lead to hypocapnia which is a deficiency of carbon dioxide in the blood. The result is respiratory alkalosis, and eventually hypoxia, or the reduction of oxygen delivery to tissue. As well as having a marked effect on the biochemistry of the body, BPDs can influence emotions, circulation, digestive function as well as musculoskeletal structures involved in the respiratory process. Essentially a sympathetic state and a subtle, yet a fairly constant state of fight-or-flight becomes prevalent. This can cause anxiety, as well as changes in blood pH, muscle tone, pain threshold, and many central and peripheral nervous system symptoms. Despite not being a disease, BPDs are capable of producing symptoms that mimic pathological processes, including gastrointestinal or cardiac problems. Musculoskeletal imbalances often exist in patients with BPDs. These may result from a pre-existing contributing factor or may be caused by the dysfunctional breathing pattern. Types of imbalances include loss of thoracic mobility, overuse/tension in accessory respiratory muscles, and dysfunctional postures that affect the movement of the chest wall, as well as exacerbating poor diaphragmatic descent.
Symptoms of Breathing Pattern Disorders (BPD)
Breathing pattern disorders manifest differently based on the individual. Some people may exhibit high levels of anxiety/fear whereas others have more musculoskeletal symptoms, chronic pain, and fatigue. Typical symptoms can include frequent sighing and yawning, breathing discomfort, disturbed sleep, erratic heartbeats, feeling anxious and uptight, or achy muscles and joints. There may also be a correlation between BPD and lower back pain.
Breathing Pattern Disorders (BPD) Treatment
Physical therapy can help with BPDs. Many patients with BPDs have coexisting musculoskeletal concerns, particularly back and neck pain. Manual therapy techniques can be used to help address issues such as increased tone or activity, elevated and depressed ribs, and alterations in the mobility of thoracic articulations. These treatments will include thoracic mobilisations, stretches, muscle energy techniques (MET), positional release, trigger point release, and integrated neuromuscular inhibition techniques. Breathing retraining will also be taught by your therapist. Exercises and lifestyle recommendations will be prescribed once there is re-established balanced breathing and improved sleep patterns. If in doubt, please seek professional physiotherapy advice in Singapore.
Physiotherapy Support for Breathing Dysfunction
Breathing patterns can affect posture, movement, and overall function. Physiotherapy may assist in addressing underlying musculoskeletal factors contributing to breathing difficulties. Visit our Physio Clinic in Singapore to learn how therapy can support breathing retraining and physical function.
Check out our popular articles: Diastasis Recti, Tight Back Muscles, Irritable Bowel Syndrome (IBS), Temporomandibular Joint (TMJ) Dysfunction, Tennis Elbow, Wrist Tendon Injury, Sciatica, Whiplash, Hernia, Herniated Disc (Slipped Disc).